Whether through social media, traditional news outlets, or word of mouth, discussions about GLP-1 therapy are everywhere. These medications, originally approved by the FDA for the treatment of Type 2 diabetes, have since been authorized for weight loss therapy and are now recommended by the American Diabetes Association as potential first-line options for both indications. With more than 42% of U.S. adults diagnosed with obesity and roughly 35 million with Type 2 diabetes, it’s no wonder the popularity of GLP-1 therapies has skyrocketed, with numerous endorsements labeling them as “miracle drugs.”
However, both doctors and patients are encountering challenges related to medication access, adherence, and insurance barriers. Health system specialty pharmacies (HSSP) play a critical role in overcoming these obstacles and improving patient outcomes associated with GLP-1 therapy.
Understanding GLP-1 Medications
GLP-1 treatment has become a cornerstone for diabetes and weight management, offering significant health benefits for patients with Type 2 diabetes and obesity. Understanding these medications, their mechanisms, and their barriers is essential to improving patient access and adherence.
What are GLP-1 Receptor Agonists?
GLP-1 receptor agonists are a class of medications that work by mimicking the body’s natural glucagon-like peptide-1 hormone. By doing so, they help regulate blood sugar levels, slow stomach emptying, and signal the brain that the body is still full.
These drugs are FDA-approved for treating Type 2 diabetes and obesity, with additional benefits for patients with heart disease or sleep apnea.
Examples of GLP-1 Agonists
Over the years, several GLP-1 agonists have been developed, each available and marketed under multiple brand names and formulations to meet different patient needs. Below are some of the most commonly used GLP-1 medications:
- Dulaglutide (Trulicity®)
- Exenatide (Bydureon® BCise™)
- Liraglutide (Saxenda®, Victoza®)
- Semaglutide (Ozempic®, Rybelsus®, Wegovy®)
- Tirzepatide (Mounjaro®, Zepbound®)
These medications differ in their dosing schedules, mechanisms of administration, and specific indications, but all work the same to improve blood sugar levels and support improved long-term health outcomes.
What are the Barriers to GLP-1 Access and Adherence?
Despite their benefits, GLP-1 medications present unique challenges at a national level.
During the COVID-19 pandemic, drug manufacturers struggled to keep up with demand. Even those able to produce the medications faced difficulties acquiring the necessary injection devices. These challenges led to widespread shortages across nearly the entire class of GLP-1 medications. As their popularity continues to rise, retail, mail-order, and specialty pharmacies alike are still struggling to fulfill patient prescriptions, despite recent supply chain improvements.
Additionally, patients often opt to discontinue this medication due to issues such as intolerance, loss of insurance coverage, affordability concerns, or pharmacy shortages.
Access Issues
Shortages and insurance barriers create major obstacles for patients needing GLP-1 medications. Common access challenges include:
- High demand and limited supply: While shortages in many areas of the U.S. have improved, the popularity of GLP-1 medications has led to widespread shortages, making it difficult for patients to obtain their medication, even when they have a prescription.
- Insurance barriers: While some insurance plans cover GLP-1 therapies, navigating the processes of step therapy and prior authorization can be overwhelming for patients. Doctors’ offices understand these processes but often face heavy workloads, which can slow down prior authorization submissions and approvals.
- Lack of patient education or awareness: Many patients are unaware of how these medications work, how to manage side effects, or how to navigate the complexities of insurance coverage.
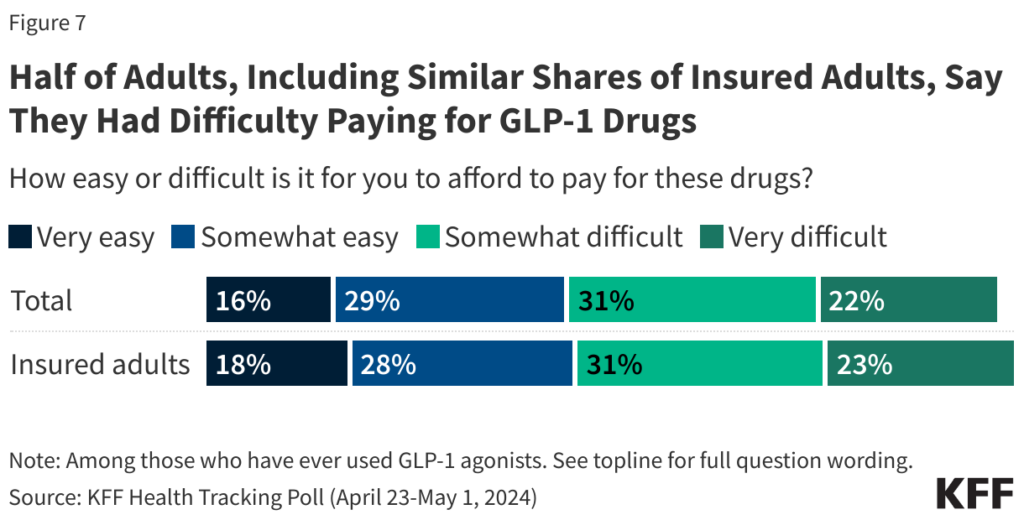
- Affordability concerns: Out-of-pocket costs can be prohibitively high. KFF research found that 54% of adults who have taken GLP-1 drugs reported difficulty affording the therapy, with 22% stating it was “very difficult.”
- Geographic disparities: Patients in rural or underserved areas tend to face significant disparities in accessing GLP-1 therapies. These individuals often have limited access to specialty providers and pharmacies equipped to dispense these medications. Farther distances to travel and fewer local care options can lead to delays in treatment and hinder positive health outcomes.
Adherence Barriers
Even after overcoming access barriers and obtaining the medication, many patients struggle with adherence. A recent study from Prime Therapeutics found that nearly half of patients discontinue GLP-1 therapy within the first year, and three out of four stop treatment by year two. Discontinuation rates are higher among lower-income groups, those with multiple health conditions, and patients over 65.
Research identifies several reasons for these high rates, including:
- Patient perception of injectable medications: Many patients are hesitant about self-administering injections, a barrier that some are unable to overcome. This is due to a combination of fear of self-injection, even with an auto-injection device, as well as the stigma many living with diabetes have that moving to injections means they have “failed.”
- Managing expectations for results: Patients may stop treatment if they don’t see immediate weight loss results, whether based on expectations of rate or extent of weight loss.
- Side effects: Gastrointestinal issues such as nausea, vomiting, and diarrhea are common and often lead to discontinuation.
- Financial concerns: Ongoing medication costs can make long-term adherence challenging. The average out-of-pocket cost for GLP-1 medications ranges from $900 to $1,200 per month without insurance coverage, while in-network costs for patients with insurance can vary significantly, often falling between $25 to $200 per month, depending on the plan and copay assistance programs. These financial barriers can discourage continued therapy adherence.
- Psychological barriers: Some patients experience frustration, get discouraged, or have anxiety related to treatment expectations and results, leading to nonadherence.
“Approximately one in five patients discontinued GLP-1RA therapy within the first 12 months and only half were adherent.”
https://pubmed.ncbi.nlm.nih.gov/39215626/
How Specialty Pharmacy Improves Patient Access and Adherence to GLP-1 Receptor Agonist Medications
While GLP-1 receptor agonists are not traditionally classified as “specialty” medications, integrating them into an HSSP model offers several advantages. Unlike traditional retail or mail-order pharmacies, HSSPs are directly connected with healthcare providers and electronic health records (EHRs), allowing them to streamline medication access and adherence.
Medication Access Solutions
Health system specialty pharmacies help patients access GLP-1 medications, particularly those who face financial, logistical, or insurance-related barriers. These medication access solutions help patients navigate complex coverage requirements, obtain financial assistance, and adhere to their prescribed treatments. They do so by:
- Facilitating insurance approvals and navigating prior authorizations: HSSPs work directly with insurance companies to reduce treatment delays.
- Coordinating with manufacturers for patient assistance programs: HSSPs can connect patients with financial assistance resources to lower out-of-pocket costs.
- Personalizing prescription coordination: Specialty pharmacies streamline communication between providers, insurers, and manufacturers to ensure patients receive their medications without unnecessary delays.
Patient Adherence Solutions
Maintaining long-term adherence to GLP-1 medications is essential for achieving optimal health outcomes. Health system specialty pharmacies provide comprehensive support to help patients stay on track with their treatment plans. To improve long-term treatment adherence, HSSPs offer:
- Patient education on injection techniques and expected outcomes: Specialty pharmacists provide training on proper administration and realistic weight loss expectations. Many programs now offer hands-on injection training sessions, digital video tutorials, and real-time pharmacist support to improve patient confidence.
- Proactive follow-ups for dose adjustments and side-effect management: Patients who receive continued pharmacist-led support are more likely to stay on their treatment plan. A randomized trial study involving 8,822 older adults found pharmacist-led interventions significantly improved medication adherence.
- Data-driven adherence tracking: By leveraging technology, specialty pharmacies can monitor patient progress and intervene as soon as potential adherence barriers arise. This helps patients receive medication refills on time and properly manage their side effects.
Conclusion: Streamlining GLP-1 Access and Adherence
As the national shortage of GLP-1 medications begins to ease, pharmacies are improving access to these life-changing treatments. However, not all pharmacies are equipped to handle ongoing access challenges. A typical pharmacy often relies on extensive back-and-forth communication, resulting in dozens of faxes between the pharmacy, the provider’s office, and the insurance company. Patients are left waiting during this time, unsure when they will receive their medication.
Shields’ integrated specialty pharmacy care model minimizes these inefficiencies. By streamlining communication and insurance approvals, partnering with Shields can help improve time to therapy to 24-48 hours while working to reduce out-of-pocket costs for patients. With dedicated support from a team of passionate clinical pharmacists and proven patient adherence solutions, your patients can be confident to start, continue, and benefit from their GLP-1 therapy.
Looking for more?
Check out our white paper, Analysis of Glucagon-Like Peptide-1 Agonist Trends Within An Integrated Health System Specialty Pharmacy, on how an integrated pharmacy model improves adherence and reduces out-of-pocket costs for GLP1 drugs.